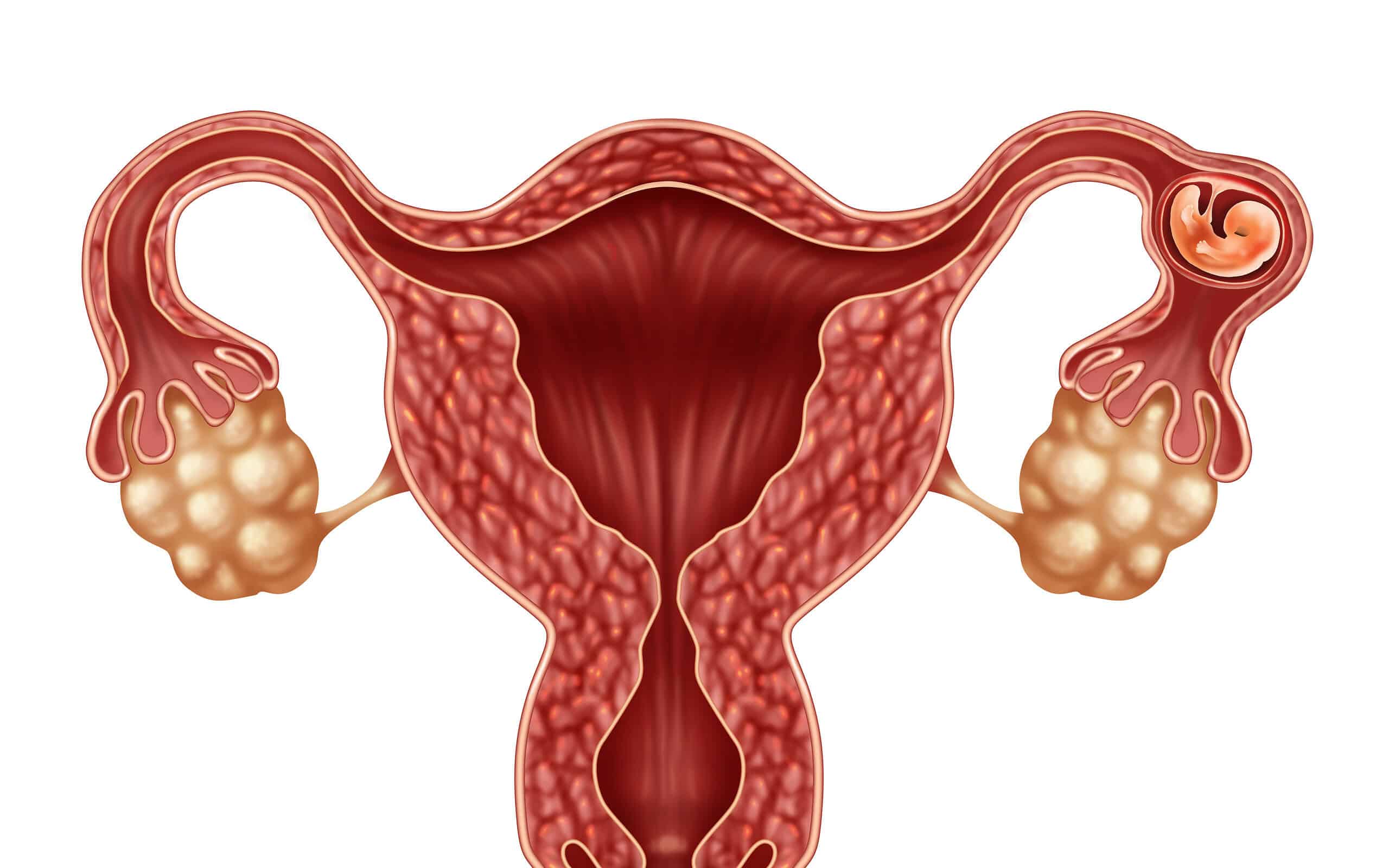
An ectopic pregnancy is one in which the fertilized egg attaches itself to a place other than inside the uterus. Almost all (more than 95 percent) ectopic pregnancies occur in a fallopian tube; hence the term “tubal” pregnancy. Rarely, the egg may implant elsewhere, such as in the abdomen, ovary, or cervix. Because the narrow fallopian tubes are not designed to hold a growing embryo, the fertilized egg in a tubal pregnancy cannot develop normally. Eventually the walls of the fallopian tube stretch to the point of bursting. If this happens there is a very real danger of life-threatening hemorrhaging.
| Ectopic Pregnancy Breakdown | |||
| Symptoms | Diagnosis | Treatment | Life After |
During the 1980s, the rate of ectopic pregnancy increased, affecting about seven of every 1,000 reported pregnancies in the United States. Even so, death from ectopic pregnancy is rare, occurring in fewer than one of every 2,500 cases. Advanced detection techniques have contributed to this low fatality rate. Read on to learn more about the symptoms, diagnosis, and causes of ectopic pregnancies.
Key Points
- Ectopic pregnancies occur went the egg attaches outside of the uterus, typically in the fallopian tubes.
- Symptoms can vary for each woman but include pain in the abdomen, pelvis, or shoulder as well as vaginal bleeding, gastrointestinal issues, or dizziness.
- Surgical removal of the ectopic pregnancy is the typical treatment, however, in some cases, methotrexate may be used to dissolve the ectopic pregnancy.
- Regular follow-up visits following the ectopic pregnancy are necessary to monitor hCG levels.
What Causes Ectopic Pregnancy and Who's at Risk?
Most cases of ectopic pregnancy are caused by an inability of the fertilized egg to make its way through a fallopian tube into the uterus. This is often caused by an infection or inflammation of the tube, which has caused it to become partly or entirely blocked. Scar tissue left behind from a previous infection or an operation on the fallopian tube may also hinder the egg's movement. Previous surgery in the pelvic area or on the tubes can also cause adhesions (bands of tissue that bind together surfaces inside the abdomen or the tubes). A condition called endometriosis, in which tissue like that normally lining the uterus is found outside the uterus can also cause blockage of a fallopian tube. Another possible cause is an abnormality in the shape of the tube, which may be caused by abnormal growths or a birth defect.
Most ectopic pregnancies occur in women 35 to 44 years of age. The major risk factor for ectopic pregnancy is pelvic inflammatory disease (PID). This is an infection of the uterus, fallopian tubes, or ovaries. The risk of ectopic pregnancy is higher if a woman has had:
- A previous ectopic pregnancy.
- Surgery on a fallopian tube.
- Several induced abortions.
- Infertility problems or medication to stimulate ovulation.
What are the Symptoms of Ectopic Pregnancy?
In many cases, a pregnant woman and her doctor may not at first have any reason to suspect an ectopic pregnancy. The early signs of pregnancy, such as a missed period and other symptoms and signs, also occur in ectopic pregnancies.
Pain is usually the first sign of an ectopic pregnancy. The pain may be in the pelvis, abdomen, or even the shoulder and neck (due to blood from a ruptured ectopic pregnancy building up under the diaphragm). Pain from an ectopic pregnancy is usually described as sharp and stabbing. It may come and go or vary in intensity. Additional warning signs of ectopic pregnancy include vaginal bleeding, gastrointestinal symptoms, and dizziness or light-headedness.
Although there may be other reasons for any of these symptoms, they should be reported to your doctor.
How is Ectopic Pregnancy Diagnosed?
If your doctor suspects an ectopic pregnancy, she or he will probably first perform a pelvic exam to locate pain, tenderness, or a mass in the abdomen. Your care provider may order lab tests, the most useful of these being the measurement of hCG. In a normal pregnancy, the level of the hCG hormone approximately doubles about every two days during the first 10 weeks. In an ectopic pregnancy, however, the rate of this increase is much slower. An hCG level that is lower than what would be expected for the stage of the pregnancy is one reason to suspect an ectopic pregnancy. The hCG level may be tested several times over a certain period to determine whether it is increasing at a normal rate.
Progesterone is another hormone that can be measured to help in the diagnosis of ectopic pregnancy. Low levels of the hCG hormone may indicate that a pregnancy is abnormal. Further tests will be needed to confirm whether the pregnancy is ectopic and, if it is, where it is located.
Ultrasound exams may also be used to help determine whether a pregnancy is ectopic. With this technique, a device called a transducer, which emits high-frequency sound waves, is moved over the abdomen or inserted into the vagina. The sound waves bounce off internal organs and create an image that can be viewed on a TV-like screen. With this procedure, your doctor may be able to see whether the uterus contains a developing fetus.
A procedure called culdocentesis is occasionally used to aid in diagnosing ectopic pregnancy. This technique involves inserting a needle into the space at the very top of the vagina, behind the uterus, and in front of the rectum. The presence of blood in this area may indicate bleeding from a ruptured fallopian tube.
What's the Treatment for Ectopic Pregnancy?
Treatment of ectopic pregnancy usually consists of surgery to remove the abnormal pregnancy. Surgery is generally scheduled soon after an ectopic pregnancy is diagnosed. At one time, a major operation was needed for ectopic pregnancy. General anesthesia was used, and the pelvic area was opened with a large incision. Now, however, it is often possible to remove an ectopic pregnancy with a less extensive technique called laparoscopy.
In this procedure, a small incision is made in the lower abdomen, near or in the navel. The surgeon then inserts a long, thin instrument, called a laparoscope, into the pelvic area. This instrument is a hollow tube with a light on one end. Through it, the internal organs can be viewed and other instruments can be inserted. Sometimes a second small incision is made in the lower abdomen, through which surgical instruments can be placed. The laparoscope allows the surgeon to remove the ectopic pregnancy and repair or remove the affected fallopian tube. Laparoscopy may be performed possibly with local anesthesia but more likely with regional or general anesthesia.
A fallopian tube that has ruptured from an ectopic pregnancy usually must be removed. Less extensive surgery can be done if the ectopic pregnancy has been found early before the tube has been stretched too much or has burst. In these instances, it may be possible to remove the ectopic pregnancy and repair the tube, allowing it to continue to function. Occasionally, a medication called methotrexate can be used to dissolve an ectopic pregnancy. This medication may be used either with or without laparoscopy, depending on how far the pregnancy has developed.
What About the Future After an Ectopic Pregnancy?
After treatment for an ectopic pregnancy, your doctor will want to see you on a regular basis to recheck your hCG level until it reaches zero. An hCG level that remains high could indicate that the ectopic tissue was not entirely removed. If this is the case, you may need additional surgery or medical management with methotrexate.
The outlook for future pregnancies after an ectopic pregnancy depends mainly on the extent of the surgery that was done. Although the chances of having a successful pregnancy are lower if you've had an ectopic pregnancy, they are still good – perhaps as high as 60 percent – if the fallopian tube has been spared. Even if one fallopian tube has been removed, an egg can be fertilized in the other tube. If you've had one ectopic pregnancy, though, you're more likely to have another one. If you've had an ectopic pregnancy, talk to your doctor before becoming pregnant again so that together you can plan your care.
The content of this article should not be considered professional medical advice. Exercise due diligence when seeking relevant health information. Always consult your healthcare provider before making any medical decisions.
The image featured at the top of this post is ©Lightspring/Shutterstock.com